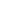Intrauterine insemination
Fertility treatments - Intrauterine insemination
With intrauterine insemination, fertilisation occurs within the mother's body, in contrast to in vitro fertilisation.
We can distinguish two types of intra-uterine insemination: homologous and donor.
Homologous or artificial insemination
Homologous (or artificial) insemination means that intrauterine insemination is done using the partner's sperm. Unlike IVF, then, fertilisation occurs in the mother's body in this case, not in the laboratory. Indications for insemination are light to moderate sperm quality disorders.
At the point when the woman ovulates, we receive sperm cells from the man in the laboratory, which are processed. We call this process sperm washing. The good, motile sperm cells are isolated and concentrated. Then the sperm cells are put into a liquid containing a lot of nutrients to ‘activate' them. The concentrated, activated sperm is then introduced to the woman's womb through her vagina using a small catheter.
Traditionally, the female partner is given medicine to gently stimulate her ovaries at this point, in order to have a perfect egg cell at the time of insemination. During stimulation, ovulation is induced using Pregnyl®. We know that administering this medicine leads to ovulation 37 to 40 hours later. In this way, we can identify the ideal time for optimal fertility, at which point the sperm cells can be introduced. Thus this stimulation considerably increases the chances of effective fertilisation.
Insemination by donor
For insemination by donor, we use cells from an anonymous or known sperm donor. Unlike homologous insemination, therefore, the partner's sperm is not used.
This technique is used (for obvious reasons) with single women who wish to have children or lesbian couples. However, it can also be used for heterosexual couples where the man has no sperm cells at all (called ‘azoospermia'). Azoospermia can exist from birth, for example due to a chromosomal disorder, or acquired, for example due to an undescended testicle, infections of the testicle or male sterilisation.
A very strict screening procedure is applied to sperm donors. Obviously, we screen for infectious diseases (hepatitis B, hepatitis C, HIV, syphilis, chlamydia etc.), but also for genetic and/or family conditions. Moreover, the sperm cells are tested for resistance to freezing and survival after freezing and thawing, after which they are in fact frozen for a quarantine period. The donor is only accepted by the tissue bank as a sperm donor once he has passed through all these stages and as long as he meets all the requirements. The sperm cells are frozen for storage in the tissue bank.
Jan Palfijn General Hospital has its own, Belgian sperm bank.